We perform the semen analysis according to guidelines of the WHO-2010 manual.
The following factors are valued in a semen analysis:
Volume of the ejaculated matter:
About 90% of semen volume is made up of secretions from the accessory glands, mainly the prostate and seminal vesicles, with minor contributions from the bulbourethral (Cowper’s) glands and epididymides. This reflects the secretory activity of the glands.
The lower reference limit for semen volume is 1.5 ml. Low semen volume is characteristic of obstruction of the ejaculatory duct or congenital bilateral absence of the vas deferens, a condition in which the seminal vesicles are also poorly developed.
Low semen volume can also be the result of collection problems (loss of a fraction of the ejaculate), partial retrograde ejaculation or androgen deficiency.
High semen volume may reflect active exudation in cases of active inflammation of the accessory organs, an excessively long sexual abstinence period or due to hypertrophia of the seminal vesicles.
Color:
A normal liquefied semen sample has a homogeneous, grey-opalescent appearance.
It may appear less opaque if the sperm concentration is very low. A green or yellowish color indicates seminal infection. Brown, redish or other dark colors indicate the presence of blood (haemospermia), generally due to an inflammation or congestion in any level of the seminal path.
Viscosity:
If the seminal liquid is thick, it can inhibit the forward movement of the sperm cells.
This problem is solved by getting semen prepared for intrauterine inseminations.
pH:
The pH of semen reflects the balance between the pH values of the different accessory gland secretions, mainly the alkaline seminal vesicular secretion and the acidic prostatic secretion. pH alterations in semen indicate further alterations in the prostate or seminal vesicles.The lower reference limit for pH is 7.2.
Number of spermatozoids:
The terms “total sperm number” and “sperm concentration” are not synonymous.
Sperm concentration refers to the number of spermatozoa per unit volume (cc or ml) of semen and is a function of the number of spermatozoa emitted and the volume of fluid diluting them. The concentration of spermatozoa in the semen, while related to fertilization and pregnancy rates, is influenced by the volume of the secretions from the seminal vesicles and prostate and is not a specific measure of testicular function.
The lower reference limit for sperm concentration is 15 × 106 spermatozoa per ml.
The total number of spermatozoa per ejaculate and the sperm concentration are related to both time to pregnancy and pregnancy rates and are predictors of conception.
The number of spermatozoa in the ejaculate is calculated from the concentration of spermatozoa, which is measured during semen evaluation.
For normal ejaculates, when the male tract is unobstructed and the abstinence time short, the total number of spermatozoa in the ejaculate is correlated with testicular volume and thus is a measure of the capability of the testes to produce spermatozoa and the patency of the male tract.
The lower reference limit for total sperm number is 39 × 106 spermatozoa per ejaculate.
Sperm cell mobility:
The motility of each spermatozoon is graded as follows:
• Progressive motility (PR): spermatozoa moving actively, either linearly or in a large circle, regardless of speed.
• Non-progressive motility (NP): all other patterns of motility with an absence of progression, e.g. swimming in small circles, the flagellar force hardly displacing the head, or when only a flagellar beat can be observed.
• Immotility (IM): no movement.
The lower reference limit for progressive motility (PR) is 32%.
The lower reference limit for total motility (PR + NP) is 40%.
The total number of progressively motile spermatozoa in the ejaculate is of biological significance. This is obtained by multiplying the total number of spermatozoa in the ejaculate by the percentage of progressively motile cells.
Sperm cell vitality:
Sperm vitality, although may be determined routinely on all samples, but is especially important for samples with less than about 40% progressively motile spermatozoa. This test can provide a check on the motility evaluation, since the percentage of dead cells should not exceed the percentage of immotile spermatozoa. The percentage of viable cells normally exceeds that of motile cells.
It is clinically important to know whether immotile spermatozoa are alive or dead. Vitality results should be assessed in conjunction with motility results from the same semen sample. The presence of a large proportion of vital but immotile cells may be indicative of structural defects in the flagellum; a high percentage of immotile and non-viable cells (necrozoospermia) may indicate epididymal pathology. The lower reference limit for vitality is 58%.
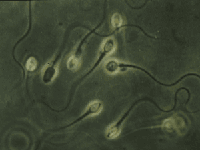
Sperm cell morphology:
The analysis of sperm morphology is subjective and particularly difficult to standardize, since it attempts to draw an artificial cut-off point between normal and abnormal cells, on the basis of a multitude of characteristics of sperm heads and tails.
Human semen samples contain spermatozoa with different kinds of malformations.
By the strict application of certain criteria of sperm morphology, relationships between the percentage of normal forms and various fertility endpoints (time-to-pregnancy (TTP), pregnancy rates in vivo and in vitro) have been established, which may be useful for the prognosis of fertility.
The lower reference limit for normal forms is 4%.
Agglutination:
This phenomenon takes place when sperm cells get stuck together and, thus, lose mobility.
It can be caused by antisperm antibodies, by a big sperm cell concentration or by infections.

Leukocytes:
Leukocytes, predominantly polymorphonuclear leukocytes, are present in most human ejaculates The reference value is 1.0 × 106. If there is an increase in the number of leukocyes, a semen culture with an antibiogram will be conducted in order to diagnose the cause and the most adequate treatment using antibiotics.
